T1D Guide
T1D Strong News
Personal Stories
Resources
T1D Misdiagnosis
T1D Early Detection
Research/Clinical Trials
Ketones Crash Course: 3 Things Every T1D Needs to Know
Whether you were just diagnosed or you’ve lived with type 1 diabetes (T1D) for decades, ketones are one of those topics everyone thinks they understand — until they don’t. Here’s what actually matters when it comes to ketones, diabetic ketoacidosis (DKA), and when it’s time to head to the ER.

1. DKA vs. Nutritional Ketosis
Yes, both involve ketones — but they are very different physiological states, driven by very different causes.
In nutritional ketosis, ketones form because the body is burning fat for fuel when carbohydrate intake is very low. This can happen on ultra-low-carb or ketogenic diets and occurs in the presence of enough insulin. Ketone levels in nutritional ketosis are typically low to moderate and fall within a relatively safe range for most people.
General ketone ranges (blood ketones):
- 0.0–0.5 mmol/L: Normal
- 0.6–1.5 mmol/L: Elevated
- 1.6–3.0 mmol/L: High
- ≥3.0 mmol/L: Urgently high and concerning for DKA
While nutritional ketosis usually stays below 3.0 mmol/L, ketone levels at or above 3.0 mmol/L meet diagnostic criteria for DKA when accompanied by insulin deficiency and acidosis.
Low-level ketones driven by diet are generally considered safe as long as insulin is present and you’re not sick, dehydrated, or insulin-deficient. However, illness, dehydration, missed insulin, vomiting, or certain medications (such as SGLT-2 inhibitors) can push ketones higher and faster — even if blood sugar isn’t extremely elevated.
For example, if you’re sick with little appetite, your healthcare provider may recommend drinking fluids with carbohydrates or eating small snacks to prevent starvation ketosis from progressing in a body already under stress.
By contrast, elevated ketones caused by insufficient insulin, illness, vomiting, or dehydration are a different and more dangerous situation. These ketones can rise rapidly, disrupt your body’s acid-base balance, and become life-threatening without prompt treatment.
It’s also important to know that high blood sugar alone does not cause DKA. DKA is driven primarily by absolute or relative insulin deficiency. High blood sugar often occurs alongside DKA, but it is not the main trigger — lack of insulin is.
.jpg)
Ginger’s real-life example:
In my mid-20s, I ate an ultra-low-carb diet for about six months — basically bacon, greens, and broccoli cooked in bacon fat. On urine strips, I tested “moderate” (that magenta color we all know). But on a blood ketone meter? I was only 1.2 mmol/L. No big deal. No danger — because I knew my ketones were diet-driven. Context is everything. With my healthcare team’s support, I continued managing my glucose levels with daily insulin therapy.
2. Signs & Symptoms of DKA
When ketones build up in your blood to high enough levels, your blood becomes acidic, which can make you very sick and can be life-threatening. The sooner you recognize the signs and symptoms of DKA, the sooner you can take action.
Because DKA can develop quickly — sometimes in a day or less — it’s important to develop a DKA or ketone management plan with your healthcare team ahead of time. This includes knowing when and how to check ketones, how to give correction insulin, how to stay hydrated, and when to recheck levels.
While some early steps can be managed at home using your care plan, contact your healthcare provider or seek emergency care if symptoms worsen, ketones remain high, or you’re unable to keep fluids or insulin down. DKA is not something to wait out, and getting help early can prevent serious complications.
Common signs and symptoms of DKA include:
- Very high blood sugar levels
- Medium or large ketones in your urine or blood, using at-home test strips
- Feeling extremely thirsty
- Needing to pee a lot
- Dry mouth or dry skin
- Feeling very tired or weak
- Repeated nausea or vomiting
- Stomach pain
- Fast or deep breathing
- Breath that smells like sour fruit or nail polish
- Trouble thinking clearly or feeling confused

If you have type 1 diabetes and notice these symptoms, don’t wait. DKA is an emergency, and getting help quickly can save your life.
First, call your healthcare team. If they are unreachable and you are experiencing vomiting combined with other symptoms, consider visiting the emergency room for intravenous fluids and insulin.
The longer you stay home trying to treat it yourself, the more likely you’ll be in severe DKA by the time you do go to the hospital. The sooner you go to the ER, the more likely you will prevent DKA. Treating DKA in the hospital can take a day or several. Preventing DKA with a bag of intravenous fluid only takes a few hours — then you go home. It’s worth the trip.
Ginger’s real-life example:
In my mid-20s, I caught a brutal stomach bug. I tried to rehydrate at home so I didn’t “waste” a trip to the ER. Huge mistake. I kept just enough fluids down to think I was making progress, then drank too much, puked it all up, and ended up even more dehydrated. I needed electrolytes, fluids, and that metabolic buffer — and I could’ve saved myself hours of misery by going sooner. Now? I don’t wait. If a stomach bug hits, I’m heading to the ER.
3. Pump Site Failures & When It’s Time for the ER
Pump site failures are annoying, but they can also be dangerous. A kinked cannula, bad adhesive, or a set that just didn’t take can cause your insulin delivery to stop completely. And since pumps deliver rapid-acting insulin only, that means you’re suddenly running on zero basal insulin. Ketones can develop within hours.
But not every pump issue requires an ER trip. If you catch it early, swap the site, give injected insulin, hydrate, and see your numbers respond, home troubleshooting is totally reasonable. Watch your ketones, watch your blood sugar, and check again in an hour or two.
The ER becomes necessary when things aren’t improving. If you’ve changed the site, taken injected insulin, and your blood sugar stays sky-high — or your ketones stay moderate to large — that’s a big red flag. Add symptoms like nausea, vomiting, stomach pain, rapid breathing, or exhaustion, and you shouldn’t wait it out. A pump failure can go from “weird high” to DKA surprisingly fast.
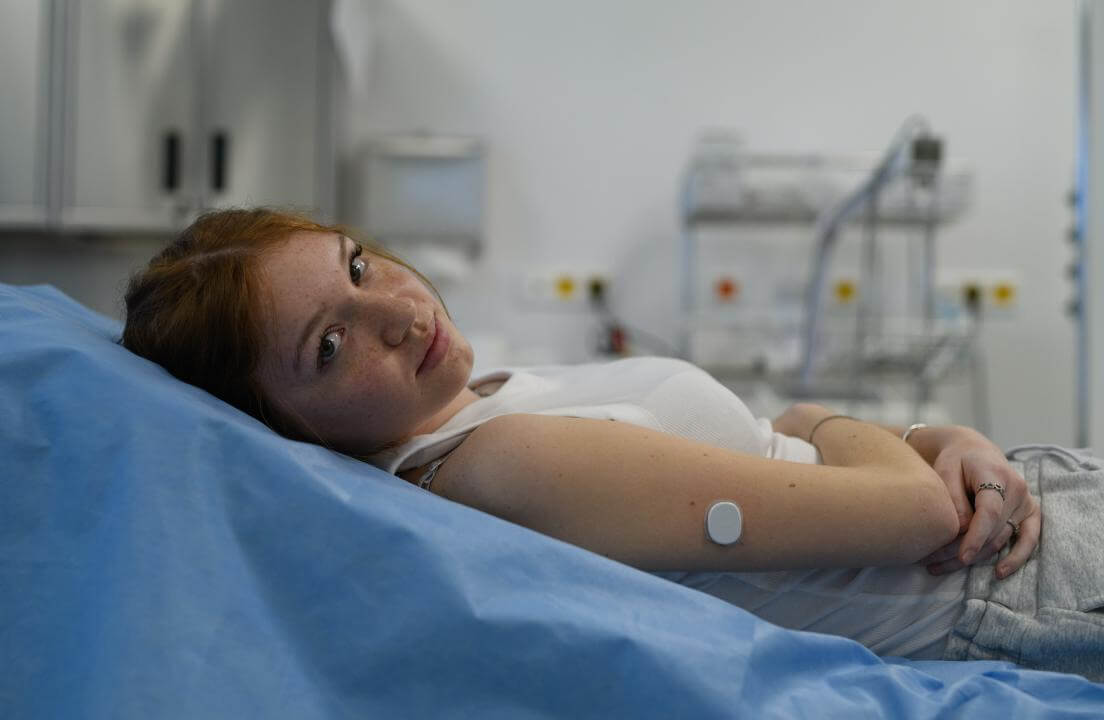
Ginger’s real-life example:
Back in 2003 — no CGMs, no internet resources — I spent a winter night stringing Christmas lights outside the movie theater where I worked. It was about 10 degrees out. The cold destroyed the insulin in my pump, but I had no idea. By morning, I was vomiting and convinced I had the flu. I spent hours trying to rest it off. By the time we called my doctor, I was deep in DKA and felt like I was dying. There was no stomach bug. It was just frozen insulin and a pump failure that could never have been managed at home.
Bottom Line
Ketones are no joke. They can go from “meh” to an emergency faster than you expect. When in doubt, get checked out. A short ER visit for IV fluids, electrolytes, and monitored insulin can prevent a days-long battle with full-blown DKA.








.webp)

.webp)
.jpg)


.jpeg)




.jpg)









.jpg)

.jpg)
.jpg)
.jpg)
.jpg)

.jpg)

.jpg)
.jpg)

.jpg)
.jpg)
.jpg)

.jpg)

.jpg)

.jpg)
.jpg)



.jpg)



.jpg)




.jpg)
.jpg)

.jpg)
.jpg)


.jpg)
.jpg)
.jpg)
.jpg)
.jpg)
.jpg)
.jpg)

.jpg)
.jpg)

.jpg)



.jpg)
.jpg)
.jpg)

.jpg)

.jpg)














.jpg)


.jpg)








.webp)