T1D Guide
T1D Strong News
Personal Stories
Resources
T1D Misdiagnosis
T1D Early Detection
Research/Clinical Trials
A Conference that Bridges the Gap Between Diabetes and Mental Health
The connection between diabetes and mental health is no longer controversial. Most people living with diabetes understand, at least intuitively, that the daily demands of management affect mood, stress levels, relationships, and self-perception. What remains less clear is how to move from awareness to meaningful support.
.jpg)
The Diabetes and Mental Health (DMH) Conference was created to address that gap. Now in its fourth year, the fully virtual event brings together mental health professionals, diabetes specialists, and individuals living with diabetes for two days of focused education and conversation.
This year’s conference will take place May 1 and 2, with all sessions recorded and available for replay through the end of July.
T1D Strong spoke with the conference founder, Allison Nimlos, a licensed marriage and family therapist (LMFT), Certified Diabetes Care and Education Specialist (CDCES), and a person living with type 1 diabetes for 32 years, about why this event exists and why it continues to grow.
Why the DMH Conference was Created
When asked about the conference's origin, Allison pointed to a pattern she noticed long before launching it.
“When I was speaking at different diabetes events, people either wanted a really broad overview of mental health and diabetes, or they wanted one very specific, deep dive topic,” she said. “I didn’t feel like either of those options allowed for both breadth and depth.”
The idea solidified during the COVID-19 pandemic, when conferences rapidly moved online, and accessibility barriers were temporarily lowered. Rather than waiting for in-person events to return, she saw an opportunity to build something new.
“With conferences moving online, the barrier to entry felt more manageable,” she said. “I wanted a space where we could cover multiple intersections of diabetes and mental health without oversimplifying or narrowing it too much.”
The first conference came together in four months. It has continued every year since.
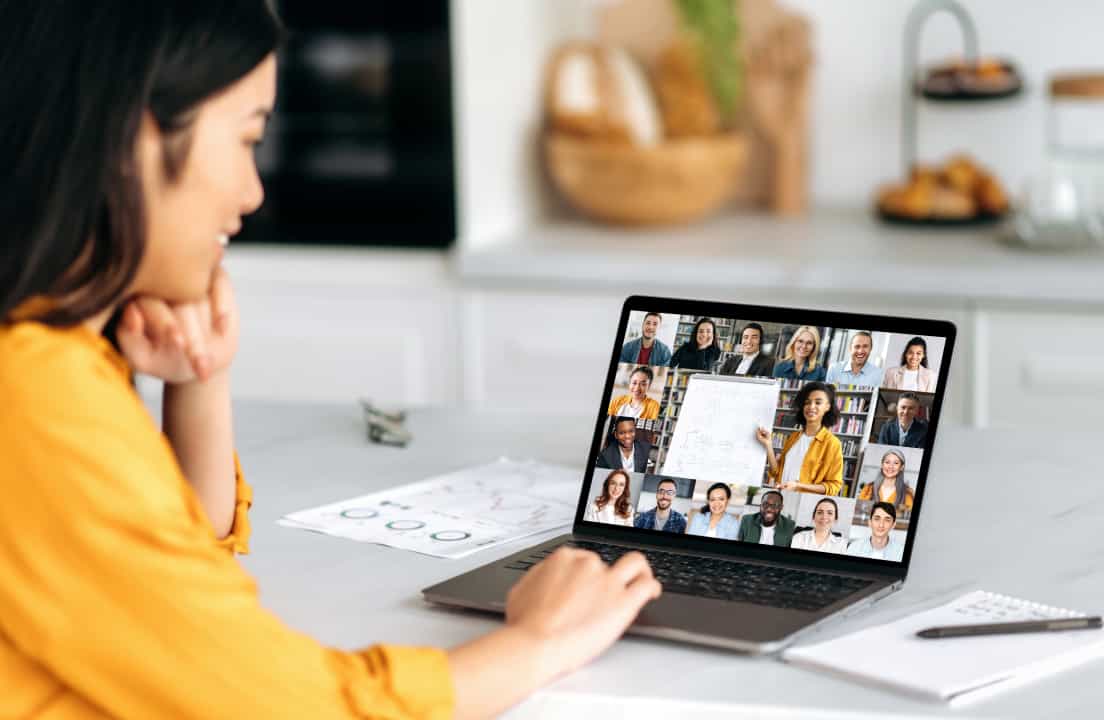
Accessibility is not an afterthought
Although in-person events have returned, the DMH Conference remains virtual by design.
“There are cost and location limitations with in-person events,” Allison said. “I’m a mom of three. It’s hard to just up and go. I know I’m not the only one in that situation. We will probably always keep this conference online,” she said. “It allows people who wouldn’t otherwise be able to attend to participate.”
Virtual access eliminates the need for flights, hotel costs, and time away from work or family. Many people with diabetes (PWD) lack the disposable income for in-person events. With the DMH Conference, attendees can log in from home, manage responsibilities, and revisit sessions later through recordings.
The event’s affordability compared to traditional conferences broadens access, especially for those facing financial strain due to chronic illness. General tickets are just $40 before May 1, 2026. For continuing education credit (CEU), tickets are $225 before May 1, 2026.
Similar conferences often cost hundreds or even over a thousand dollars after you add everything up—sometimes more.
Moving Mental Health and Diabetes Beyond Awareness
Today, few people need convincing that diabetes affects mental health. The greater challenge is implementation—not just talking about it but mobilizing action. “I don’t think people are shocked anymore when we say diabetes impacts mental health,” Allison said. “What’s missing is what we actually do about it.”
In clinical settings, mental health conversations are often unpredictable. Screening is not universal, and follow-up varies. Many PWD report that when mental health is discussed at all, they are the ones who initiate the conversation.
That needs to change—it should be more proactive, like other aspects of health. That’s where the conference hits hard. “We need to ask how we are implementing changes in care,” Allison said. “What are we actually doing in the clinic? What are therapists doing differently?”
The conference includes a strong continuing education component for mental health professionals and healthcare providers. At the same time, all sessions are open to everyone. A person living with diabetes can attend provider-focused sessions, and providers can join community-centered discussions.
“We don’t restrict sessions,” Allison said. “Everything is open. The CE track just allows providers to get credit if they need it.”
Topics that need ongoing recognition in mental health
Some subjects return year after year because they remain pressing.
“We always try to include eating disorders in some capacity,” Allison said. “We always try to address communication and stigma. Diabetes distress is another essential topic.”
.jpg)
Eating disorders and body image concerns disproportionately affect PWD. Stigma continues to shape how people experience workplace interactions, school environments, and even medical appointments. Diabetes distress, distinct from clinical depression, remains under-recognized despite its impact on daily management.
These topics are not trends. They are persistent realities.
Addressing emerging trends in diabetes care
While certain themes are consistent, the conference evolves to reflect cultural and medical shifts. This year, one of the new topics is the mental health impact of GLP-1 medications.
“You can’t go on social media without seeing ads for GLP-1s,” Allison reflected. “The way providers talk about weight loss and these medications affects body image and relationships with food.”
As these medications gain visibility, conversations around management are changing. Addressing them within a mental health framework allows for nuance rather than a reactive response. Technology and data management also remain central to the conference’s theme.
Allison says continuous glucose monitors (CGMs) and insulin pumps provide critical data but can also amplify anxiety or perfectionism: “We always get interested in technology and data and how that’s showing up emotionally.”
The Mental Load of Diabetes
Some of the most anticipated sessions this year include keynote addresses from Laura Pavlakovich of You're Just My Type, Dr. Tricia Tang, with the University of British Columbia, and Rob Howe of Diabetics Doing Things.

The mental load is the constant cognitive effort required to manage an unrelenting disease—one that offers no breaks and little forgiveness or support, even when you’re an excellent self-manager.
“Even as a single person with diabetes, you’re trying to figure it out,” Allison explained. “Add being a parent or having a high-stress job, and it’s a lot.”
This year's panel on "The Mental Load of Diabetes" features several outstanding leaders in the diabetes community who live with diabetes while managing demanding professional roles and family life. Their discussion will center on sustaining long-term health while carrying significant responsibility. “They’re running major organizations and managing diabetes at the same time,” Allison said. “I’m really excited to talk about how they juggle that mental load.”
Participating on the panel are:
- Aaron Kowalski, CEO of Breakthrough T1D—living with T1D for 40 years
- Laura Syron, President & CEO of Diabetes Canada—living with type 2 diabetes (T2D) for 10 years
- Beth Braun, Licensed Psychologist—living with T1D for 47 years
- Manny Hernandez, CEO of The Diabetes Link—living with latent autoimmune diabetes in adults (LADA) for 24 years
.jpg)
Filling a resource gap: Mental health is still under addressed
Access to mental health care remains a barrier for many.
“There aren’t a lot of therapists who specialize in diabetes,” she said. “Mental health access globally is still limited by cost, insurance, and location.”
While telehealth has expanded options in recent years, systemic challenges remain. The conference cannot replace therapy, but it can provide practical strategies and education that attendees can implement immediately.
“My hope is that someone attends a session and gets something they can apply to how they’re living right now,” Allison said.
Sessions this year include topics such as sex and intimacy with diabetes, ADHD and diabetes management, stigma, eating disorders, and provider communication. The goal is to create room for conversations that might not happen during regular doctor visits.
Mental health support is individual for people with diabetes
In addition to professional education, the conference creates community.
“There are a lot of different levels of support people can try,” Allison said. “Talking to your healthcare team is important. Therapy can be important. Community can also be powerful.”
For individuals who have experienced burnout without a language for it, simply hearing others articulate similar experiences can be transformative.
“When we see burnout, providers sometimes treat it like an education issue, as if people just don’t know better,” she said. “That’s not the case.”
Validation changes how people engage with care. It changes how they interpret their numbers. It changes how they talk to themselves.

Why Attend the DMH Conference?
When asked why someone with diabetes should go, her answer was based on practical reasons.
“Mental health services for diabetes can be hard to come by,” Allison said. “I hope this conference fills in some of that gap by providing time and space to talk about issues people don’t often get to discuss.”
For providers, the conference offers continuing education grounded in real-world clinical application. For people living with diabetes, it offers tools, language, and perspective.
All sessions are recorded and accessible through the end of July. Attendance on May 1 and 2 is not required to benefit.

Mental Health is always a Part of the Bigger Picture with Diabetes
Managing diabetes is constant and all-consuming. It affects friendships, jobs, being a parent, close relationships, who you are, and how you see yourself. Ignoring the emotional side of it doesn’t make the problems go away. Instead, it pushes them deeper inside.
The DMH Conference exists because mental health is important to include in diabetes care. It's not something optional. If we want long-term health, we need to talk about emotional well-being. This conference makes sure that conversation happens in a clear, research-based, and easy-to-access way.








.webp)

.jpeg)


.webp)

.jpg)






.jpg)




%20(1).jpg)





.jpg)

.jpg)
.jpg)
.jpg)
.jpg)
.jpg)

.jpg)

.jpg)

.jpg)
.jpg)

.jpg)
.jpg)

.jpg)
.jpg)
.jpg)


.jpg)

.jpg)


.jpg)
.jpg)



.jpg)



.jpg)

.jpg)



.jpg)
.jpg)
.jpg)

.jpg)
.jpg)


.jpg)

.jpg)
.jpg)
.jpg)
.jpg)
.jpg)
.jpg)

.jpg)
.jpg)

.jpg)



.jpg)
.jpg)
.jpg)
.jpg)


.jpg)
.jpg)









.webp)