T1D Guide
T1D Strong News
Personal Stories
Resources
T1D Misdiagnosis
T1D Early Detection
Research/Clinical Trials
Bill’s Story: A Later-in-life Type 1 Diabetes Diagnosis that Led to Gluroo
There’s a particular kind of disorientation that comes with a type 1 diabetes (T1D) diagnosis in adulthood. It doesn’t fit the narrative most people have been told—arriving in childhood with a clear identity. Instead, it slips into a life already in motion.

For Bill Sheppard, Head of Business at Gluroo, the signs were there—weight loss, excessive thirst, subtle shifts that are easy to explain away when life is busy. It wasn’t until after a school event, standing in the kitchen with his wife, that things came into focus.
“In retrospect, typical story,” he said. “I had been losing weight, had been thirsty, and all the usual things.”
His wife, a physician, suggested that he check his blood sugar. The number that came back—around 400 mg/dL—didn’t leave room for doubt. “That’s kind of instant diagnosis,” he said.
Even then, the diagnosis didn’t unfold as many expected. There was no immediate rush into insulin therapy. Instead, his early management looked deceptively simple.
A Long Honeymoon: Diabetes Management Began Simply for Bill
For the first couple of years, Bill managed his diabetes with diet and exercise. No insulin, pump, or continuous glucose monitor (CGM) alarms interrupting his sleep.
But “simple” doesn’t mean easy.

“I wasn’t thrilled about that all the time because I liked my carbs,” he admitted. “But it definitely made me… I had not been a particularly eager workout person, and this kind of forced some discipline.”
That discipline came with trade-offs. If he wanted flexibility with food, he felt like he had to earn it through movement. It was a quiet negotiation happening every day.
“If I wanted to have tastier things, then I had to work out that day.”
Like many adults diagnosed later in life, Bill experienced a prolonged honeymoon phase in which his body continued to produce some insulin. That phase stretched for years, softening the transition but not removing the reality of what was ahead.
Eventually, insulin became necessary. Multiple daily injections (MDI) followed, and diabetes moved from something he could manage around to something that required constant attention.
From Fingersticks to Full Throttle Diabetes Management
Bill’s background in technology shaped his approach to diabetes from the beginning. He wasn’t content with guesswork. Bill wanted data. At the time of his diagnosis in 2013, CGMs weren’t readily available in the United States, so he found another way.

“I had a colleague in Germany where it was available,” he said. “So I had him buy half a dozen of them every few months and ship them to me.”
That decision changed everything.
“Just the difference between fingersticks and a CGM was incredible,” he said. “Having all that data and knowing what was going on between meals and overnight and how different foods impacted things.”
Fingersticks gave him moments while a CGM gave him context. It turned isolated numbers into patterns and trends that he could actually learn from.
“And since then, I’ve looked to technology as a way of managing diabetes.”
Diabetes Technology Isn’t Perfect
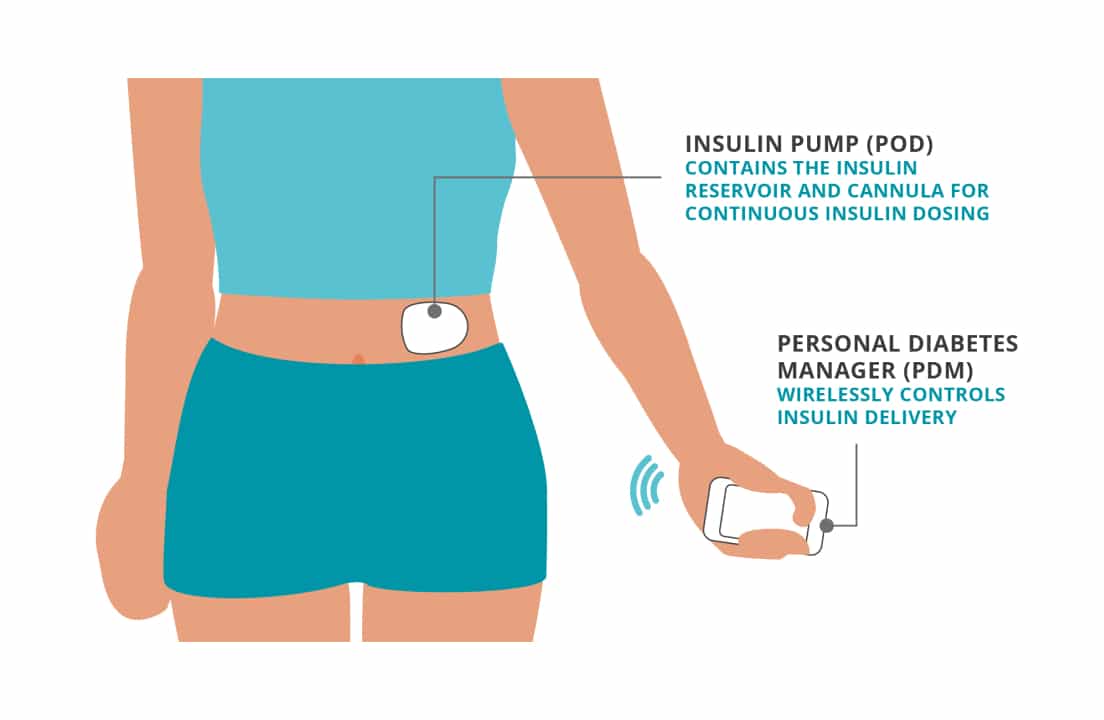
As his management evolved, so did his tools. After years on injections, Bill transitioned to an insulin pump, eventually using the Omnipod 5. Like many people aiming for tighter control, he found that automation had its limits.
“It was great at night because I didn’t have to worry about things,” he said. “But during the day, it was just not keeping me near my target.”
That gap between expectations and reality is familiar to many people who use automated systems. The technology works, but not always in the way you need it to.
“So I decided to try looping.”
With his engineering background, building and managing a DIY looping system wasn’t a barrier—it was an opportunity. It offered something he hadn’t quite found elsewhere: control over the details.
“There’s an incredible amount of detail, numbers, and knobs to deal with,” he said. “So it took a while to get dialed in.”
But for Bill, that level of customization was worth it.
Family History with Type 1 Diabetes
Bill wasn’t the first in his family to live with T1D. His brother had been diagnosed decades earlier, also as an adult.
“He was probably 30, give or take, when he was diagnosed,” Bill said. “And no other diabetes in the family whatsoever.”
That shared experience became a point of connection, especially early on.
“He referred me to his endo… who was much more aggressive with understanding what’s happening with new therapies.”
Over time, their roles shifted. Bill’s deep dive into technology eventually positioned him as the one bringing new ideas to the table.
“At some point, I became the one who was discovering more about some of the ways of managing things,” he said. “And by then he had been into it for 30 years, so you kind of get set in your habits.”
It’s a dynamic that reflects something broader in the diabetes community: experience matters, but so does evolution.
Bill’s choice to step into the healthcare world
After decades in the tech industry, Bill made a shift that brought his personal and professional worlds together. He joined Gluroo, a diabetes management platform designed to improve how people share and understand their data.

“I had never kept it a secret that I have diabetes,” he said. “So there wasn’t a concern about being more public with that.”
What surprised him wasn’t the overlap between his life and his work—it was how much he didn’t know about the healthcare system he was stepping into.
“I came in knowing a lot about type one and the various therapies and technologies,” he said. “But didn’t have any idea how much I didn’t know… about the business model, how healthcare works, who gets paid, and what the incentives are.”
That learning curve came with some frustration.
“A technology or a product that creates better outcomes or that saves money—you would think that that would be of interest,” he said. “But insurance companies often get paid by how much they bill, not by how strong the outcomes are.”
The Cost of Staying Alive with Type 1 Diabetes
For many people living with T1D, the barriers aren’t just clinical—they’re financial. Bill experienced that firsthand.
During a period when he relied on marketplace insurance, the costs added up quickly.
“It was $500 a month kind of thing if I was to just do everything the way the plan was set up.”
So he found another workaround.
“I have a niece who was in school in Canada, so I would have her buy insulin over the counter and bring it back,” he said. “It just… again, nonsensical that I could buy over the counter as an American for $40, the insulin that my insurance company here wanted to charge $500 for.”
This is a frustration many diabetes advocates and community members share within the U.S. In 2023, a report from the American Diabetes Association (ADA) estimated the annual cost of diabetes at $412 billion.
Building Diabetes Tools that Actually Help
Gluroo started with a specific purpose: helping caregivers stay connected to their loved ones’ diabetes management. That foundation still matters, but the platform has expanded far beyond it.
“We have about 210,000 users today,” Bill said. “Of that, roughly 40% are type 1, about 50% are type 2.”
The app now supports a wide range of users, from parents managing a child’s care to adults tracking their own data to individuals focused on weight loss and metabolic health.
At its core, the goal is the same: reduce friction and make data usable.
“The less friction you have in logging your food, the more likely you are to do it,” Bill said.
That’s where newer features, like AI-powered food recognition, come into play.
“You can just take a picture… and in three or four seconds, it tells you what you most likely just ate and the likely carbs and protein.”
Even with occasional inaccuracies, the system performs better than most people can estimate on their own.
“It’s actually more accurate than everyone except dieticians who have a scale,” he said.
Walking the Line with AI in Healthcare
As AI becomes more integrated into diabetes tools, the line between helpful and risky gets thinner. Gluroo has taken a cautious approach, particularly when it comes to offering guidance.
“We are not a regulated FDA-regulated application,” Bill explained. “We’ve been careful not to provide medical advice.”
That means certain features—like a bolus calculator—aren’t included, even though they could be useful.
“We likely would need to be regulated if we put in a bolus calculator,” he said.
Instead, the app provides supporting information, leaving the final decision to the user.
It’s not always the most convenient approach, but it’s intentional.
“You should always consult a medical provider and use the first-party apps,” he said. “Don’t rely on Gluroo for alarms that you’re going low.”
Reducing the Diabetes Noise for Gluroo Users
If there’s one thing people with diabetes don’t need, it’s more noise. More alerts and data can create more friction for people with diabetes who want fewer redundancies across their technology and apps.
Gluroo’s goal is the opposite.
“By trying to make sure the experience is as streamlined as possible… you don’t have to think too much about what you’re doing,” Bill said.
That simplicity is backed by something much more complex: data.

“We now have over 12 billion CGM readings from our users and more than 30 million food log entries.”
That scale creates opportunities to uncover patterns that individuals might miss on their own.
“To the extent that we have all this data and we can use that to help discover patterns and convert that into potential insights—that’s a big part of it.”
It even opens the door to addressing broader issues, such as misdiagnosis.
“We’ve been approached about using that data to help identify type 2s who may actually be type 1s,” he said.
Type 1 Diabetes: a Professional and Personal Evolution
Bill’s journey with T1D didn’t start in childhood or follow a “predictable” path. Bill’s journey with T1D busts a misconception that most new cases of T1D occur in childhood, but according to the ADA, over half of all new cases occur in adults over the age of 18.
While there are many things you can do to manage diabetes well, it still involves a degree of unpredictability and uncertainty, as reflected in many community members' experiences.
Bill’s professional and personal journeys with diabetes haven’t stopped evolving.
“We've recently launched a paid app, GotCGM,” Bill said. The team is excited to see what the future holds for its impact on the diabetes community.
From early management without insulin to DIY looping, from importing CGMs to working inside a diabetes tech company, Bill’s experience reflects something many people with T1D understand deeply: there is no static version of “figuring it out.”
“I’m constantly learning,” he said.
Maybe the best place to find yourself is not in having all the answers but in simply moving forward.








.webp)

.webp)



.jpeg)

.jpg)




%20(1).jpg)




.jpg)
.jpg)
.jpg)

.jpg)
.jpg)

.jpg)
.jpg)
.jpg)
.jpg)
.jpg)
.jpg)

.jpg)
.jpg)
.jpg)
.jpg)

.jpg)

.jpg)


.jpg)
.jpg)

.jpg)

.jpg)
.jpg)


.jpg)
.jpg)

.jpg)
.jpg)
.jpg)
.jpg)
.jpg)

.jpg)
.jpg)
.jpg)
.jpg)
.jpg)
.jpg)

.jpg)
.jpg)

.jpg)
.jpg)
.jpg)

.jpg)
.jpg)


.jpg)
.jpg)
.jpg)













.jpg)


.jpg)















.webp)