T1D Guide
T1D Strong News
Personal Stories
Resources
T1D Misdiagnosis
T1D Early Detection
Research/Clinical Trials
Early T1D Detection: Mom Screens Toddler, Stage 2 Diagnosis Offers Critical Head Start
Diabetes was never a concern. The Marions had no family history, but when their son started showing classic type 1 diabetes symptoms, Hannah Marion acted quickly to get their 21-month-old screened. They caught the illness in stage 2, before life-threatening side effects, and today Hannah says early testing was the best decision she could have ever made.

Hannah Marion and her husband, Andrew, are the proud parents of two young sons, Beckham (three) and Carter (five). Though they have no family history of type 1 diabetes (T1D), Hannah does have Hashimoto’s thyroiditis and celiac disease, two conditions closely related to T1D. People with type 1 are two to four times more likely to develop Hashimoto’s, while 1-16% of T1D patients also have celiac.

A Stage 2 Diagnosis that Changed Everything
Hannah, who lives with her family in Mount Washington, Kentucky, was in nursing school when she learned about the textbook symptoms of type 1 diabetes. When her youngest son, Beckham, just 21 months old, began showing signs, she knew she had to act.
Key Signs of T1D
- Excessive Thirst: Intense, unquenchable thirst.
- Frequent Urination: High volume of urination, including bedwetting in children
- Rapid Weight Loss: Unexplained weight loss, often with high hunger levels.
- Extreme Fatigue: Extreme exhaustion, weakness, and lack of energy.
- Blurred Vision: Temporary changes in vision due to fluid changes in the eye.
- Increased Hunger: Constant hunger despite eating
“Internally, I kept saying “check, check, check” to each symptom as it matched Beckham’s perfectly - which is odd considering stage 2 is typically asymptomatic.”
Beckham was diagnosed with stage 2 type 1 diabetes. We now know that type 1 has three stages, and there are benefits to catching the disease in its earlier phases. The main reason is to avoid the life-threatening side effect of diabetic ketoacidosis (DKA).

Hannah had never heard about the stages of type 1 diabetes, but as she did more research, she thought that it may correlate to Beckham’s clinical presentation.
Decision to Screen
Hannah knew something was wrong, but Andrew needed some convincing that Beckham had T1D. Hannah brought up concerns with her pediatrician, who tested Beckham in the doctor’s office.
“Beckham’s blood sugar was 150 three hours after eating,” said Hannah. “This was enough to raise some eyebrows, but not to warrant an immediate trip to the emergency room.”
Additionally, Beckham was not losing weight; however, he had not gained any weight for many months. He was vomiting frequently and experienced extreme thirst and recurrent urination.
“Our pediatrician ordered an A1c and other bloodwork, but not autoantibody testing for type 1.”
In the meantime, Hannah bought an over-the-counter glucometer and began testing Beckham’s blood glucose levels at random. “During this time of waiting for the lab work, I had received readings up to 240, so I knew there was cause for concern.”
However, Beckham’s pediatrician called back a few days later and reassured them that all the lab work looked fine; he did not see the need for a referral to an endocrinologist.
Hannah was not convinced.
“I knew normal levels from nursing school, and I knew the dangers of DKA, so I reached out to the Autoimmunity Screening for Kids (ASK) program to screen him for autoantibodies.”

ASK is a free, Denver-based research initiative that screens children aged 1-17 for type 1 diabetes and celiac disease.
Initially, he was positive for three of four autoantibodies, but on recheck, he was positive for all four.
“He has bounced back and forth on having the IA-2 antibody, but most recently tested positive for it at 45.”
Since Beckham was just a toddler, he remained largely unaware of everything going on, the continuous glucose monitor (CGM) changes, finger pricks and bloodwork, which Hannah found to be a small comfort. Though it was bittersweet, she took solace in knowing he wouldn’t recognize any difference.

Additionally, knowing it made it easier to monitor for signs of dysglycemia (erratic blood sugar changes) before he could articulate how he felt.
A Simple Test, A Life-Changing Result
The screening process for Beckham was incredibly easy once Hannah was in touch with the ASK program. The kit was self-explanatory, and the blood draw at their local LabCorp went very well. However, the hardest part of the screening process was the waiting, said Hannah.
“I hated receiving the positive results indicating T1D, but it also helped explain so much. Other than that, it was the best decision I could have ever made for Beckham.”
Clinicians from the ASK program sent Beckham a Dexcom CGM to wear to gather data.
They also drew another set of labs to verify their findings. They recommended that the Marions proceed with transferring Beckham’s care to an endocrinologist, despite him still being in stage 2.
Hannah later screened herself and their other son, Carter, through her son’s endocrinologist.
“Carter’s autoantibody results were deemed negative, but he does have IAA at 0.005 and ZnT8A at 0.002, so we will continue to watch, given that there was some level of autoantibody.”
A Positive Experience and Outcome
Today, Beckham uses an insulin pen when needed and wears a Dexcom G7 CGM constantly to monitor his blood sugar levels.
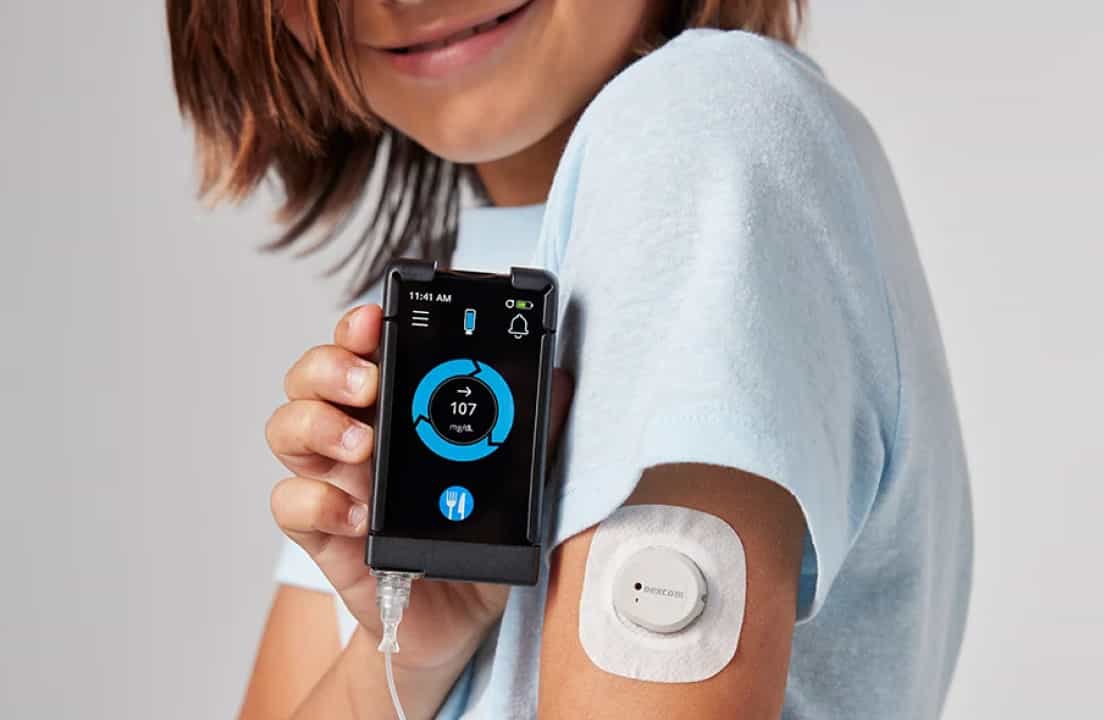
At age three, he’s still in stage 2, but occasionally hits 400+, where the Marions dose insulin to bring him down.
Hannah was surprised by the coordination of care she received through ASK and by the ability to draw so many conclusions from the lab work.
“I appreciated the level of information shared with me once the results came in, and was in awe of the fact that I received a phone call so quickly, ensuring his results were promptly addressed,” said Hannah.
“In my previous experiences with abnormal lab work, it seemed that there could be other explanations. However, with positive autoantibody results, it was very definitive.”
ASK told the Marions that with the number of autoantibodies, Beckham has a 100% risk of developing stage 3 type 1 diabetes within his lifetime, more than likely within the next 10 years.
“We were also told he has a significant risk of developing it within the next five years. We are a year and a half into the journey with stage 2.
ASK also told the Marions about immune-modifying therapies like Tzield, but not much was shared, given he was underage. Tzield (teplizumab-mzwv) delays the onset of stage 3 type 1 diabetes by a median of approximately two years (roughly 24 to 25 months) in patients with stage 2 T1D. The FDA recently expanded the approval of Tzield to include children as young as 1 year old with stage 2 T1D.
Why Early Detection Matters
When T1D is detected early through screening, it transforms a sudden, life-threatening emergency into a manageable, monitored condition. Also, early intervention creates opportunities to protect the remaining insulin-producing beta cells, providing time for education, specialized care and clinical trials.
One moment that stayed with Hannah was when she heard, “He has type 1 diabetes, not full-blown, but he does have it.”
“This was a moment of realization for me, and also helped erase these odd feelings that I don’t necessarily belong to the group of parents with a type 1 child, just because we caught it early,” Hannah said. “Additionally, it has helped improve my skills as a future nurse by showing me that the early stages exist, so I can look for them in the patients I see.”
Screenings Impact on Care & Planning
“The ability to 'sit' with the results and prepare myself for a type 1 diabetic child was one aspect of screening that I am eternally grateful for,” said Hannah. “I have seen DKA in the hospital setting, and I have witnessed how overwhelmed the parents seem while trying to take in such a large amount of information.”
Learning the information slowly, over time, has been so beneficial,” said Hannah. “It’s also helped me prepare for how we want to manage Beckham’s type 1 diabetes.”
A Less Invasive Diagnosis
“Screening my child made me aware of catching things earlier and advocating for my child,” Hannah added. “I gained confidence in my 'mom intuition,' and even if the screening was negative, I feel it would still have taught me the importance of advocating for what is best for my child.”
“The effects of screening and doing lab work were far less invasive than what a DKA diagnosis would have been.”
.jpg)
Additional studies show that children diagnosed with DKA may struggle with their blood sugar levels and have higher A1Cs than children not diagnosed with diabetic ketoacidosis.
“Being able to prepare for the future of the disease’s progression has led to a much easier transition for my son and has offered long-term benefits for his emotional well-being,” Hannah said.
“I wish more people understood that it is a decision that is best for their longer-term needs. Even if screening is negative, it is reassuring to know that something so scary is checked off the list of possibilities for the near future (with consideration for future re-screenings).”
Moving forward, Beckam’s pediatrician has also stated that he will do more screenings and has even asked Hannah's perspective on the topic.
“I believe screening for T1D should be done at regular intervals as part of standard well-checks for kids. Knowing that iron and lead levels are checked, this feels like another one of those that could be checked to ensure the best outcomes for children.”
Ongoing Support
Hannah pointed out how much support the diabetes community offers. From ASK to Facebook groups, she wished she had known about them before her screening process. She has since created a Stage 1 & 2 Type 1 Diabetes Facebook page to offer assistance to this unique group who find out through screening.
T1D Scout provides an at-home, saliva-based genetic screening kit to assess a child's risk of developing type 1 diabetes (T1D) without needles. Parents can register online, receive a kit by mail, and return a saliva sample to a lab to calculate a Genetic Risk Score (GRS).


.webp)





.webp)





.jpeg)


%20(1).jpg)




.jpg)
.jpg)
.jpg)
.jpg)
.jpg)

.jpg)
.jpg)

.jpg)
.jpg)
.jpg)
.jpg)
.jpg)
.jpg)
.jpg)
.jpg)

.jpg)
.jpg)
.jpg)
.jpg)

.jpg)

.jpg)


.jpg)
.jpg)

.jpg)

.jpg)
.jpg)


.jpg)
.jpg)


.jpg)
.jpg)
.jpg)
.jpg)
.jpg)
.jpg)


.jpg)
.jpg)
.jpg)
.jpg)
.jpg)
.jpg)
.jpg)
.jpg)

.jpg)
.jpg)

.jpg)
.jpg)
.jpg)

.jpg)
.jpg)


.jpg)

.jpg)
.jpg)

.jpg)
























.webp)